The coronavirus is having a major impact on the U.S. health care system—including primary care. To track the impact of the coronavirus and what is needed to respond, the Primary Care Collaborative partnering with the Larry A. Green Center to conduct a weekly survey of primary care practices on their responses to the COVID-19 crisis. The goal of this effort is to regularly assess primary care’s ability to evaluate and manage patients in the midst of COVID-19 and to consider policy implications going forward.
Check back weekly for the latest survey results and updates.
For last week's data, see Week 1 Results.
Who replied to the survey in Week 2?
Over 500 primary care physicians, nurse practitioners, and PAs took the survey in week two. Respondents spanned an even wider cross-section of the country this week, covering 48 states plus Puerto Rico and the Virgin Islands. A third own their practice, and nearly three-quarters (72%) work at a practice with more than three clinicians. Respondents ranged among practice types, including rural (17%), community health centers (18%), and practices associated with an academic medical center (34%).
Results at a glance
Little change was seen from last week in terms of testing capabilities. 43% of respondents still report no capacity to test patients for COVID-19 at their practice; another 39% report having capacity to test based on CDC guidelines/restrictions only.
The percentage of respondents reporting “severe impact” on their practices doubled since last week. Nearly half (49%) reported that their practice was experiencing “severe impact” (the highest possible response) due to the current status of COVID-19, up from 21% the week before. Another 27% report “close to severe” impact.
The biggest stressors on practices are now: 1) reduced well/chronic visits and 2) staffing shortages due to staff illness/self-quarantine .
-
Nearly 90% of respondents report that their practice has had to limit well/chronic visits; though fewer (7%) now report sick visit availability as a problem.
-
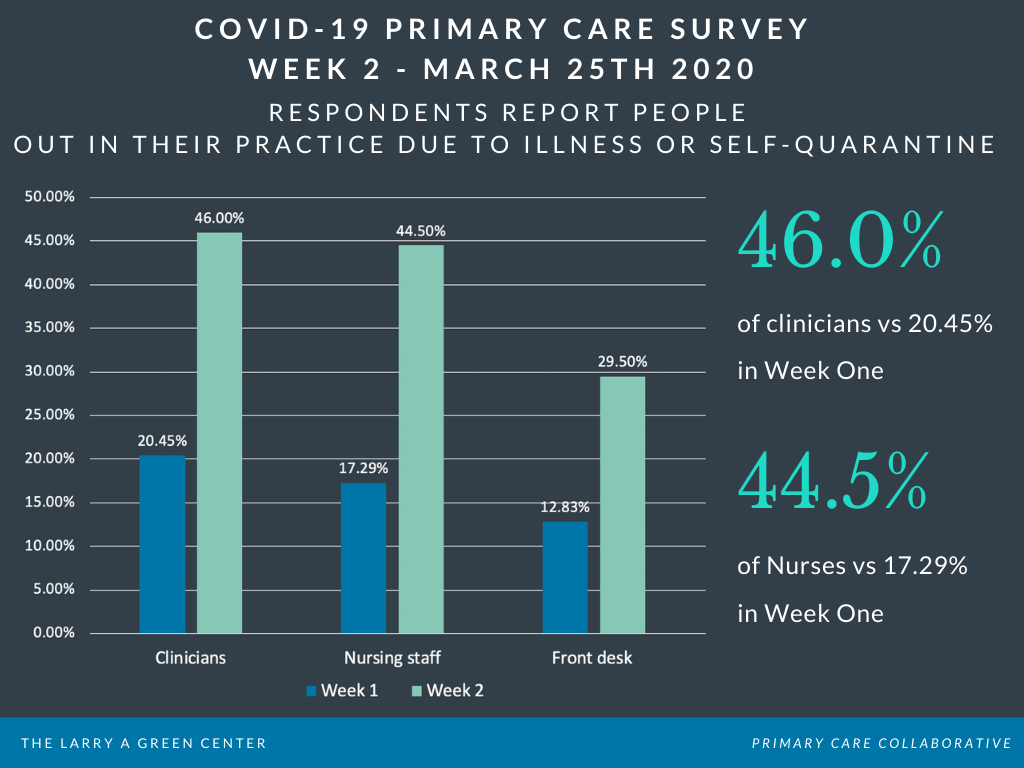
Respondents are increasingly reporting clinician/staff absences due to sickness/self-quarantine as a stressor on their practices: 46% report clinicians out; 45% report nursing staff out; and 30% report front desk staff out. Each of these percentages are double or more from absences reported in last week’s survey.
As telehealth takes a more prominent role, respondents report high patient amenability to virtual services but much less certainty on how those services will be paid for.
-
83% of respondents say patients are accepting of telehealth visits, and nearly half of respondents plan to continue using telehealth after the COVID crisis is controlled.
-
Payment for telehealth varies: 62% report that these services are reimbursable by insurance; 52% report that they are reimbursable by Medicaid.
-
A third of respondents do not know how their telehealth services will be paid for.
Still, uptake of virtual services appeared to be slow as of the close of the week 2 survey:
-
70% of respondents work at practices with NO e-visits, and 60% work at practices with NO use of video visits.
-
Over a third work at practices with NO patient portal/secure messaging.
Only 46% of respondents reported that they believe the majority (60% or more) of their office visits/contacts are reimbursable.
Voices from the Primary Care Frontlines
235 respondents in week 2 included open text comments.
Half of the comments highlighted the lack of vital supplies for clinicians as a serious concern.
“We stopped doing patient visits last Monday due to lack of PPE [personal protective equipment].” (Oregon)
“Not enough protective equipment. Front line doctors are going to die because we are being sent out to fight something we cannot see, we cannot treat, & we cannot test for without the PPE necessary to protect ourselves.” (Virginia)
Many other comments described financial strain on practices that has, or will, lead to closures.
“We are [trying] to do as much telehealth as possible to limit exposure with no idea how much or if we will get paid. Our business has dropped off immensely and we are giving away a lot of free care but are trying to remedy that with technology. I am very worried about cash flow for our small private practice.” (Colorado)
"Extreme financial strain that will impact our survival and ability to care for ANY patients for ANY reason. Nothing new, but primary care needs more resources.” (North Carolina)
"Our biggest issue right now is cash flow. Visits have [plummeted] and we are trying to avoid laying off experienced staff. We are projecting that physician owners will have zero income this year at best and may have to put money back into the practice in order to keep it viable if social distancing continues for more than 2 months.” (New York)
A few comments pointed to how practices are adapting to the evolving landscape, but with challenges:
“Our group managed to set up parking lot COVID-19 tests this week after learning we could get supplies from a commercial lab. We also started telehealth visits once the government pressed insurers to lessen restrictions.” (Pennsylvania)
“I want to know that I can do telemedicine visits and get reimbursed by insurance and how to do that. I have tried accessing webinars that are Full and feel very scared.” (Oregon)
“We have started respiratory clinics. Only 12 cases in the state. The calm before the storm. Not actually calm at all but limited [cases].” (West Virginia)
Responses to week 2 of the survey were collected March 20-23, 2020.
Learn more: Download the Executive Summary and the Executive Summary + Comments.
| Attachment | Size |
|---|---|
| 124.3 KB | |
| 124.3 KB | |
| 15.23 KB |

Are you a physician, nurse practitioner, or PA working in primary care?
Help PCC and the Larry A. Green Center track how your practice is responding to the COVID-19 outbreak by completing the Green Center's occasional survey.
The regular surveys are no longer being conducted.
COVID-19 Updates
May 9, 2022 | Primary Care Collaborative
April 19, 2022 | Primary Care Collaborative
April 19, 2022 | Primary Care Collaborative
March 7, 2022 | STAT
February 27, 2022
- 1 of 39
- next ›

Recent News
July 16, 2024
May 31, 2024
May webinar highlights: “The Commercial Market: Alternative Payment Models for Primary Care” Nate Murray explains w… https://t.co/KX9Wi2w6oY —
1 year 1 month ago
@CMSinnovates’ primary care strategy is rooted in a 2021 @theNASEM’s report which called #primarycare “foundational… https://t.co/glbPxvCysg —
1 year 1 month ago
@CMSinnovates has a new #primarycare strategy, envisioning “ACO-based primary care model tests that may focus on pr… https://t.co/aJGF1z411l —
1 year 1 month ago
- Page 1
- ››
Secondary menu
Copyright © 2024 Primary Care Collaborative